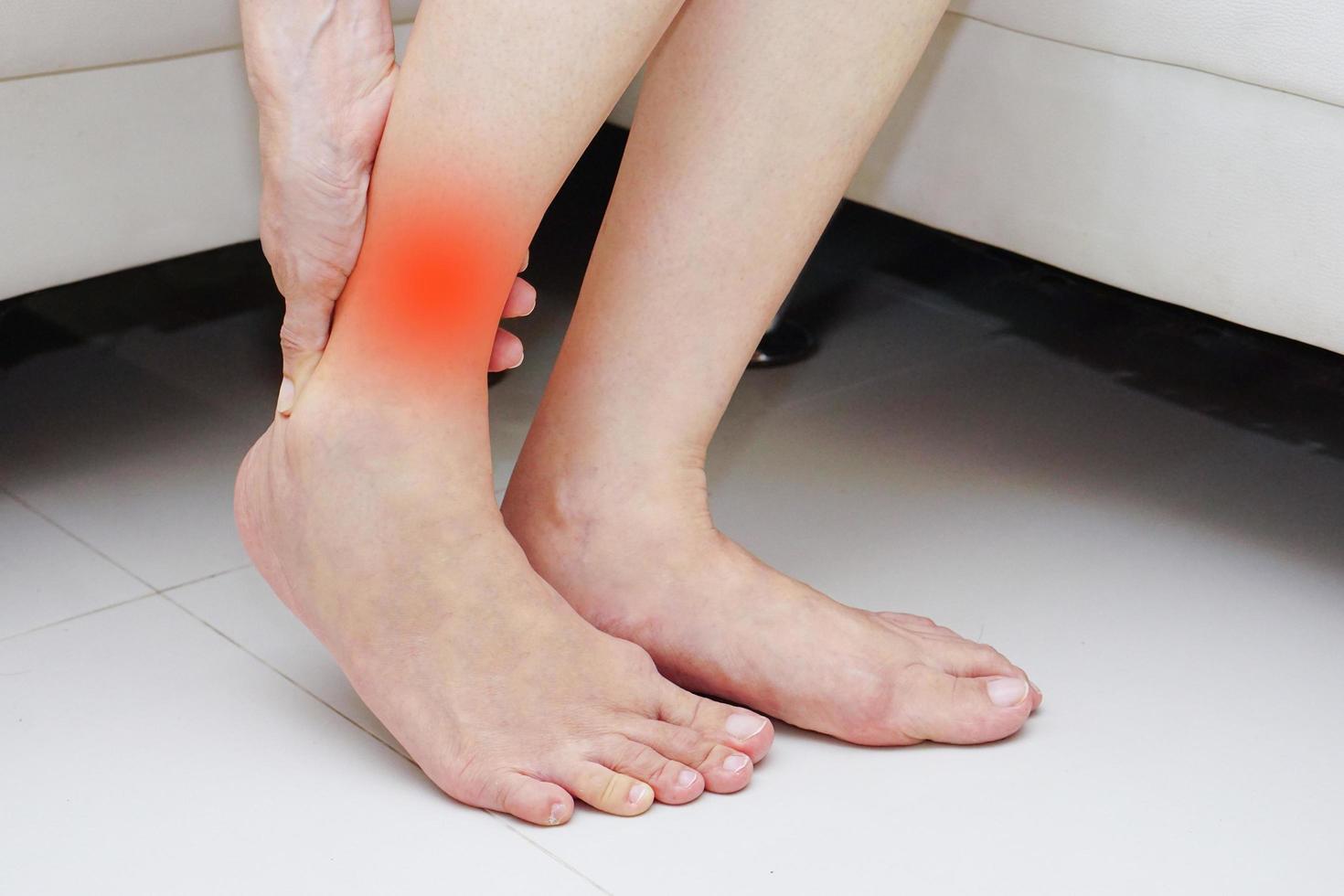
Tendon disorders such as Achilles tendon pain, tennis elbow, swimmer's shoulder, and jumper's knee affect both teenage athletes and senior exercisers. These ailments arise when a tendon is repeatedly forced beyond its normal capacity, leading to microscopic damage that gradually builds up.
"Tendons are inherently vulnerable to overuse," says Jess Snedeker, a professor of orthopaedic biomechanics at ETH Zurich and Balgrist University Hospital. "All the forces generated by our muscles are funneled through very thin, rope‑like structures that must move the skeleton. When the load becomes excessive, the tendon’s integrity is compromised."
Clinicians label this group of conditions as tendinopathies. They rank among the most frequent reasons patients visit orthopaedic clinics, yet reliable, long‑lasting treatments remain elusive. Physical therapy can ease symptoms, but severe cases often see only modest improvement. This therapeutic gap has driven researchers to search for the root molecular triggers of tendon degeneration.
HIF‑1 Identified as a Molecular Instigator
A collaborative team led by Snedeker and Katrien De Bock, professor of exercise and health at ETH Zurich, has now highlighted a single protein—hypoxia‑inducible factor‑1 (HIF‑1)—as a central player in tendon disease. HIF‑1 acts as a transcription factor, turning specific genes on or off inside cells.
Earlier work reported elevated HIF‑1 levels in injured tendons, but it was unclear whether this increase was merely a by‑product of damage or a true driver. By combining mouse experiments with analyses of human tendon samples, the researchers demonstrated that HIF‑1 does more than accompany disease; it actively initiates it.
Direct Evidence from Animal and Human Studies
In mice, the team engineered two extremes: one strain kept HIF‑1 permanently switched on, while another strain had the protein completely deactivated in tendon tissue. Mice with constant HIF‑1 activation developed classic signs of tendinopathy even without any extra loading. In contrast, mice lacking HIF‑1 in their tendons remained healthy, even when subjected to strenuous exercise that would normally cause injury.
The investigators also examined tendon cells harvested during routine surgeries. Whether from mice or humans, higher HIF‑1 levels led to abnormal cross‑linking within collagen fibers—the structural backbone that gives tendons strength. These aberrant cross‑links weaken the tissue and set the stage for chronic pain.
The Importance of Early Intervention
"Our findings not only clarify how tendinopathy starts, they also stress the value of treating it early," Snedeker notes, especially for young athletes whose tendons are still adaptable. Over time, HIF‑1‑driven damage can accumulate, eventually becoming irreversible. At that point, physiotherapy offers little benefit, and surgery may be the only option to remove the diseased portion.
Seeking Targeted Therapies
With HIF‑1 now recognized as a molecular culprit, the next logical step is to block its activity. However, De Bock cautions that HIF‑1 performs essential functions throughout the body, particularly in sensing low‑oxygen conditions. Systemic inhibition could trigger unwanted side effects.
One promising avenue is to develop drugs that silence HIF‑1 only within tendon tissue. Another strategy involves mapping the entire network of molecules regulated by HIF‑1, hoping to find downstream targets that can be safely modulated. Researchers are already exploring these pathways, aiming for precise, tendon‑focused treatments that avoid broader systemic impact.
